DISTRIBUTION OF DISCHARGES AND INPATIENT DAYS BY PAYER | 2023
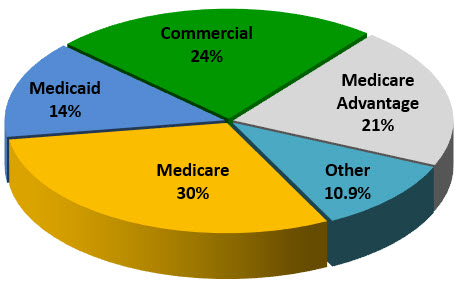
In FY2023, the Federal programs Medicare and Medicaid combined to cover over 34 percent of the discharges from community hospitals in Kansas. In addition, the number of Medicare inpatient days is 43 percent of the inpatient days in Kansas.Medicare Advantage plans now cover over 20 percent of discharges, up from 14 percent in 2018
In the Federal Fiscal Year 2023 Medicare Provider Analysis and Review (MEDPAR) data file produced by the Centers for Medicare and Medicaid Services, there were 189,644 Medicare discharges from 164 Kansas facilities. The total charges for these discharges were $9,658,114,973 and total interim payments were $1,194,023,151. The interim payment to charges ratio was 12.4 percent; the average charge per discharge was $75,559.
SOURCE: Kansas Hospital Association FFY 2023, Kansas Inpatient Database
DISTRIBUTION OF KANSAS DISCHARGES BY PAYER
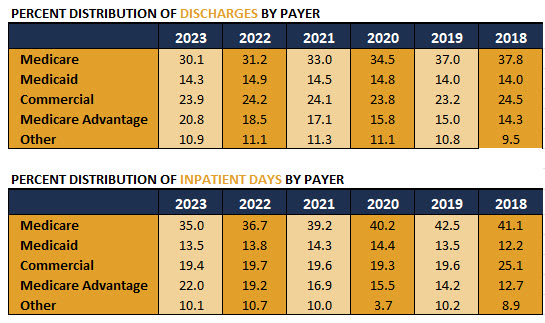
SOURCE: Kansas Hospital Association FFY 2023, Kansas Inpatient Database